|
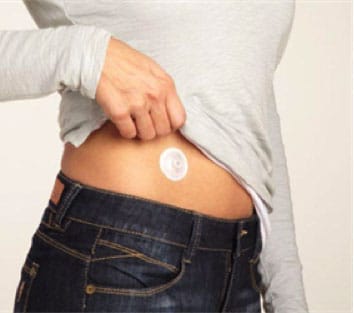
19 th November, The day when Dr.Raskar's Diabetes Clinic for the first time India launched iPort Advance in India. Insulin Management in diabetes is no more painful and Needle less Pricks.
i-Port Advance injection port lets you take your medication without having to puncture your skin for each shot. It’s easy to apply and easy to use. The port can be worn for up to three days and during all normal activities, including exercising, sleeping, and bathing.
0 Comments
The case for bitter melon in diabetes keeps looking better and better. New information and new products have come out, though there are still no large studies on humans.
To review: Bitter melon is a fruit and a vegetable, nobody can decide which. It grows in most tropical countries in Asia, Africa, Australia, South America, and the Caribbean. It goes by the names bitter melon, bitter gourd, bitter squash, karela, and goya, among many others. The scientific name is Momordica charantia. It seems to lower blood sugar well. Look at the comments to my 2013 article on bitter melon or read customer reviews for any bitter melon product such as teas or capsules. You will find overwhelming agreement that Momordicaworks. The main complaints are about taste, and some people get digestive upset, as can happen with metformin. There seems to be a risk of going too low if you take bitter melon along with certain diabetes medicines such as insulin or a sulfonylurea. There may also be a risk of going low using bitter melon along with metformin. You’ll have to proceed carefully and speak to your health-care provider if you’re on these or other medicines, as bitter melon can interact with a variety of drugs, but a number of readers commented that they lowered their doses or stopped meds completely with their doctor’s approval. How bitter melon works is not known, but at least three active ingredients have been isolated in the lab. An article in The Open Medicinal Chemistry Journal in 2011 listed multiple chemicals from bitter melon that could lower sugar. The authors believed the strongest chemical was charantin, which appears to act similarly to insulin. It gets glucose into the cells like insulin does and keeps excess glucose in the liver like insulin and metformin do. It may be that nature developed us to have more than one way to burn glucose, and bitter melon is one of those ways. How to take it My article in 2013 focused on bitter melon tea. Many readers commented that juicing a raw bitter melon worked for them. Others suggested chopping it up and nibbling the pieces for snacks, or using it in cooking. The problem with all those natural ways is the taste. Some people like it, but others hate it. Some readers asked about bitter melon capsules, which appear to work well with no taste problems. Now there are some new ways to get bitter melon. Some might be easier and tastier for you. One group of these products is called Carela. The company sent me some varieties to try, and they tasted good. The tea comes in six flavors. It is made from chopped up bitter melon mixed with tea leaves and “other ingredients.” Carela coolers are made with liquefied bitter melon and slightly sweetened with sucralose, which does not raise blood sugars or insulin levels. The coolers come in peach and cranberry flavors. Carela cofounder Daniel Casanas said it took years of work to create a good-tasting drink while maintaining the health benefits of bitter melon. The ingredients are a trade secret, so I can’t estimate the dose of Momordica you will get in each drink. One user, a woman with Type 1 named Katie Drinkwater, told me she uses Carela to supplement her insulin. She said one 12-ounce bottle lowered her sugars about 100 mg/dl over an hour. A blogger with Type 1 named Libby reported even stronger results. A cooler kept her sugars in normal range for hours even after eating a bagel and cream cheese, which she said had never happened before. Casanas believes bitter melon will be the next kale — soon, everyone will be eating it. I hope he’s right, because Momordica is one of the world’s great healers. It has been found to have powerful anti-cancer properties in mice, according to Memorial Sloan Kettering Cancer Center. One of our commenters on this site said he started bitter melon tea for glucose control and his adrenal tumor disappeared. Momordica also appears to slow the progression of HIV, the virus that causes AIDS. I wonder how such a healing plant evolved, or how we evolved to get so much benefit from it. I also wonder why so few people in the West know about it. Why there has been so little research? Hopefully there will be more soon. Carela is raising money for human studies on bitter melon at this site. Fortunately, we don’t have to wait for large studies if we don’t want to. We’ve got animal and lab studies to give us a hint, and hundreds of thousands of anecdotal reports to get us started. You can read some of these ecstatic reviews here or here or in the comments section of any bitter melon diabetes article. Try it and add your own voice to the chorus. David Spero has been a nurse for 32 years and has lived with multiple sclerosis for 25 years. He is author of two books: The Art of Getting Well: Maximizing Health When You Have a Chronic Illness (Hunter House 2002), and Diabetes: Sugar-coated Crisis – Who Gets It, Who Profits, and How to Stop It (New Society 2006). He writes for Diabetes Self-Management and Arthritis Self-Management magazines. He is a project director with New Health Partnerships: Improving care by Engaging Patients, a project of the Institute for Healthcare Improvement. Keeping blood sugar levels from rising too high after meals is one of the key goals for people who have diabetes. Now, a small new study from researchers at Weill Cornell Medical College suggests that, for obese people who have Type 2 diabetes, the order in which they eat their food may be an important tool to this end.
Earlier studies have shown that consuming whey protein prior to a meal or altering the balance of carbohydrate, fat, and protein in a meal can reduce after-meal blood sugar levels. To determine what impact the order in which food is eaten at a meal has on after-meal blood sugar, researchers recruited 11 obese people with Type 2 diabetes who were being treated with the oral medicine metformin. On two separate days a week apart, the participants were given a typical Western meal consisting of vegetables, protein, carbohydrates, and fat in the form of chicken breast, steamed broccoli with butter, lettuce-and-tomato salad with low-fat dressing, ciabatta bread, and orange juice. Blood sugar and insulin levels were checked in the morning prior to eating and again at 30, 60, and 120 minutes after the meal. For the first meal, the subjects were told to eat the carbohydrates first, followed by the protein, vegetables, and fat 15 minutes later. The following week, they were instructed to eat the protein, vegetables, and fat first, followed by the carbohydrates 15 minutes later. The researchers found that, when carbohydrates were eaten last, the participants’ blood sugar levels were significantly lower at the 30-, 60-, and 120-minute after-meal checks (29%, 37%, and 17%, respectively), and insulin levels were substantially lower as well, compared to when the carbohydrates were eaten first. “Based on this finding, instead of saying ‘don’t eat that’ to their patients,’ clinicians might instead say ‘eat this before that,” said lead study investigator Louis Aronne, MD. “While we need to do some follow-up work, based on this finding, patients with Type 2 might be able to make a simple change to lower their blood sugar throughout the day, decrease how much insulin they need to take, and potentially have a long-lasting, positive impact on their health.” Limitations of the study include its small size and a follow-up period of only 120 minutes after each meal to analyze blood sugar and insulin levels. Future studies that involve a longer follow-up to determine the full impact of food order on blood sugar levels are necessary, the authors note. For more information about the research, read the article “Food Order Has Significant Impact on Glucose and Insulin Levels” or see the study’s abstract in the journal Diabetes Care. And to learn more about preventing after-meal blood sugar spikes, see the article “Strike the Spike II,” by 2014 Diabetes Educator of the Year Gary Scheiner. Diane Fennell has been an editor at Diabetes Self-Management magazine since 2003. She is currently the Web Editor for Diabetes Self-Management E-News and DiabetesSelfManagement.com. Most likely, you knew very little about diabetes before you learned that you had it. After your diagnosis, your next few doctor visits were probably a crash course in diabetes: learning how to check your blood glucose level, inject insulin or follow a schedule for taking pills, adjust your eating habits, etc. Your doctor may also have mentioned what diabetes is and what causes it in this blitz of information, but with so much to learn at once, you may not remember what he said — or remember him saying anything at all on these topics.
It can be difficult to take in so much new information at one time, especially when you are just learning diabetes terminology and adjusting to the idea of having diabetes; many people find they miss a lot of the background information about the underlying causes of their diabetes. However, understanding how and why diabetes develops can help you to be an active member of your diabetes-care team. The two main typesDiabetes mellitus, usually referred to as just diabetes, is characterized by a high blood glucose level. There are several different types of diabetes, each with a unique underlying cause. The most common forms are Type 1 diabetes and Type 2 diabetes. Both are considered chronic diseases, meaning that once diagnosed, they don’t go away. Blood glucose levels that are higher than normal but not high enough to be diabetes are now called prediabetes. For descriptions of other types of diabetes and related conditions, see “Types of Diabetes.” Type 1 diabetes used to be called juvenile or insulin-dependent diabetes, and Type 2 diabetes was called adult-onset or non-insulin-dependent diabetes. The American Diabetes Association now favors the terms Type 1 and Type 2 diabetes, which are defined based on the underlying cause of the diabetes, not on a person’s age at diagnosis or treatment method. Type 1 diabetes Type 1 diabetes occurs when the body’s immune system launches an attack against the insulin-producing beta cells in the pancreas. Why the immune system does this is not completely understood, but it is thought that both genetics and some sort of environmental trigger are involved. Certain combinations of genes make some people more likely to develop Type 1 diabetes, but having a genetic tendency alone is not enough: Not everyone at increased risk for Type 1 develops it. For instance, in identical twins (who by definition have the exact same genetic makeup), when one twin has Type 1 diabetes, the other twin also develops it only 50% of the time. It is believed that for a genetic tendency toward Type 1 to be “expressed,” a person must be exposed to an environmental “trigger” that sets the autoimmune process in motion. Many potential triggers have been proposed, including viruses, bovine serum albumin (a protein in cow’s milk), hormones, and environmental toxins, but none have been definitively proven to lead to Type 1 diabetes. Once the process is set in motion, the immune system produces antibodies to beta cells and to insulin and begins to destroy them. (Under normal circumstances, antibodies seek out and flag harmful foreign substances within the body, such as bacteria or viruses, for destruction.) This process starts many years before diabetes is diagnosed. In fact, it’s possible to identify people at risk of developing Type 1 diabetes by checking their blood for antibodies to beta cells and to insulin. Over time, the quantity of insulin produced by the pancreas and the amount circulating in the bloodstream progressively decline. The resulting signs and symptoms of Type 1 diabetes, which include high blood glucose levels, weight loss, increased urination, hunger, and thirst, and large amounts of ketones in the blood and urine, generally occur only after a majority of the beta cells have been destroyed. In the absence of insulin, glucose in the bloodstream cannot be transferred into cells as it normally would, resulting in high glucose levels in the bloodstream and a state of “starvation” within cells. The kidneys filter the excess glucose out of the blood, causing increased urination, thirst, and dehydration. Starving cells, no longer able to use glucose for energy, begin to use fat, resulting in loss of body fat and the production of ketones (chemical by-products of fat metabolism). If not treated (with insulin) in time, the combination of high blood glucose, high levels of ketones, and dehydration can lead to a very serious condition called diabetic ketoacidosis and, potentially, death. Some people with Type 1 diabetes experience a “honeymoon” period after diagnosis, during which their pancreas regains the ability to produce insulin, and they require little or no injected insulin, but this generally lasts only a short time. Within a few months, most people have very little insulin-producing capacity and require an outside source of insulin. Type 2 diabetes Type 2 diabetes is much more common than Type 1 and has a stronger genetic link. (If one identical twin develops Type 2 diabetes, there is a 90% chance that the other one will also.) Symptoms of high blood glucose are less pronounced in Type 2 diabetes compared to Type 1 diabetes; because of this, diagnosis often occurs many years after diabetes initially develops. However, the damage starts even in the absence of acute symptoms: Blood glucose levels above normal are known to increase a person’s chances of eventually developing heart disease and other complications of diabetes. Unlike Type 1 diabetes, Type 2 diabetes is not caused by an autoimmune attack. Instead, there are usually two underlying problems: insulin resistance and inadequate insulin production. Insulin resistance is when the cells of the body have a decreased response to insulin. Under normal circumstances, when blood glucose levels are high (after eating, for example), the pancreas releases insulin into the bloodstream. Insulin then interacts with muscle cells, fat cells, and other tissues, allowing them to transport glucose into the cells to be burned for energy or stored for use later. In insulin resistance, these important messages do not get through. Remember playing “telephone” as a child, when one person would whisper a word to the person next to them, and that person would whisper what they heard to the next person, and so on down the line? By the time it got to the end of the line, the word had usually mutated to something completely unrecognizable. A similar breakdown in communication is thought to occur in insulin resistance, where the signal from insulin becomes garbled, and the cell does not respond normally, taking up much less glucose than normal. When blood glucose levels remain high, the pancreas continues to secrete more insulin to compensate for its decreased effectiveness, and eventually, blood glucose returns to the normal range. Over time, however, the pancreas loses the ability to produce enough extra insulin to compensate for insulin’s decreased effectiveness, and blood glucose levels remain high. At this point, a person might be diagnosed with diabetes or prediabetes, depending on his blood glucose level at the time of testing. The liver also plays a key role in regulating blood glucose level. It releases glucose to the bloodstream when the blood glucose level is low, and it stores glucose when the level is high. When the blood glucose level is high, insulin has the important role of signaling the liver to turn off glucose production and start storing extra glucose. But if a person is insulin resistant, the liver does not respond normally to insulin, so it continues to release glucose to the bloodstream even if the blood glucose level is already elevated, making it even higher. Treating Type 2 diabetesTreating Type 2 diabetes involves treating both underlying problems (insulin resistance and inadequate insulin production). An individual’s treatment may change over time as his degree of insulin resistance or ability to produce insulin changes. Many people still make a fair amount of insulin when they are initially diagnosed with Type 2 diabetes, so their treatment may focus mainly on decreasing insulin resistance. Ways to decrease insulin resistance include increasing physical activity, following a healthy meal plan, and losing weight (even losing as little as 10 pounds can make a difference). Certain drugs are also targeted to treat insulin resistance. Metformin (brand name Glucophage) decreases the amount of glucose made by the liver, and pioglitazone (Actos) and rosiglitazone (Avandia) make fat and muscle tissues more sensitive to insulin. Other drugs address insulin deficiency by stimulating the pancreas to release more insulin, slowing the digestion of carbohydrate in foods, affecting certain hormones involved in blood glucose regulation, or preventing the kidneys from reabsorbing glucose into the bloodstream. Using one or more of these medicines and keeping carbohydrate intake moderate and spread out over the day can help the pancreas keep up with insulin needs. Ultimately, however, it is not unusual for many people with Type 2 diabetes to eventually need to take insulin injections to supply their bodies with enough insulin. Many people with Type 2 diabetes see the progression to using insulin as a negative reflection on their ability to follow their meal plan, lose weight, or otherwise take care of their diabetes. But while there are always additional steps anyone could take to further improve their health, for most people, the need to use insulin to control their diabetes does not mean they lack willpower or the desire to take good care of their diabetes. It is simply a matter of disease progression and the decreased ability of their pancreas to continue producing supernormal levels of insulin. Not just blood glucoseDiabetes is diagnosed based on blood glucose level, and keeping your blood glucose level in a near-normal range has been shown to prevent common complications of diabetes such as eye disease, kidney disease, and nerve disease. But blood glucose level is not the only concern in diabetes. High blood pressure and high blood fats (such as cholesterol and triglycerides) often occur along with high blood glucose and can also lead to complications, including heart disease. All of these concerns — blood glucose, blood pressure, and blood fats — should be addressed in a comprehensive diabetes treatment plan for good health today and to prevent diabetes-related complications down the road. elinda O’Connell is a Diabetes Nutrition Specialist at the International Diabetes Center in Minneapolis, Minnesota, and a freelance health and science writer. Laura Hieronymus, a registered nurse and master licensed diabetes educator, is a doctor of nursing candidate at the University of Kentucky College of Nursing in Lexington, Kentucky. Over the past 40 years, there has been significant debate about the nutritional value of eggs. In the 1970s, the public was told to reduce dietary cholesterol in order to reduce the risk of developing heart disease. Since eggs are the most concentrated source of dietary cholesterol, the public was cautioned against consuming more than 1 egg per day.
Soon, the association between dietary cholesterol and heart disease was questioned heavily, and research indicated that eggs were only harmful when consumed in large quantities, at more than 1 egg per day. Fast forward 40 years. Eggs are now making a comeback as nutritious food once again. Current scientific opinion suggests that it is no longer necessary to limit dietary cholesterol intake to less than 300 mg per day (the equivalent of about 1.5 eggs per day), because there is a weak association between dietary cholesterol and blood cholesterol. Egg NutritionIn essence, there are two parts of an egg which are distinctly different from each other: the yolk and the white. The yolk is a storehouse of cholesterol, saturated fat, vitamins and minerals. One egg yolk contains 55 calories 4.5 0 grams of total fat, 1.6 0 grams of saturated fat, 184 milligrams of cholesterol, and small amounts of vitamin A, vitamin D, vitamin B6, Iron and vitamin B12. The egg white is mainly a storehouse of protein. One egg white contains 17 calories, 0 grams of total fat, 0 grams of saturated fat, 0 milligrams of cholesterol, zero 0 grams of carbohydrate, and about 4 grams of protein. In addition, the egg white contains no appreciable vitamins or minerals. Eggs and Organ HealthAre eggs safe or unsafe to eat? Most importantly, how do eggs affect your risk for long-term disease, including heart disease, diabetes and cancer? In order to answer these questions, we turn to the research. Most importantly, we must evaluate eggs from multiple perspectives, rather than simply focusing only on the connection between egg consumption and heart disease. All Cause Mortality Findings from the 2008 Physicians Health Study found that consumption of more than one egg per day resulted in a 23% increase in the risk of death from any cause (1–3). Diabetes Adults with diabetes (type 1 or type 2) are 2 to 4 times more likely to develop heart disease or stroke than nondiabetic adults. The reason for this is simple: elevated blood glucose increases the risk for all forms of cardiovascular disease, including heart attack, stroke, angina, and coronary artery disease (4). The 2008 Physicians Health Study found that people with diabetes significantly elevate their risk for all cause mortality after eating about five eggs per week (1–3). Arterial Plaque Recent studies have linked egg consumption with an increase in arterial plaque. For this outcome, researchers found that three eggs per week significantly increased arterial plaque formation in carotid arteries (5), significantly elevating the risk for heart attack. Prostate Cancer Studies have also shown that eating more than 2.5 eggs per week increases the risk for the development of prostate cancer by more than 81% (6,7). Colon Cancer Overall analysis of more than 44 studies performed in over 400,000 subjects found that the risk for gastrointestinal cancers increased linearly with increasing egg consumption. The authors found that the strongest correlation was found between egg consumption and colon cancer. Specifically, eating more than 5 eggs per week increased colon cancer risk by 42% (8). Research suggests that eggs promote the development of prostate cancer because they are high in cholesterol and choline (9–11). Cholesterol is elevated in tumor cells in all tissues, and increased blood cholesterol influences the ability of tumor cells to replicate and migrate. In other words, increasing blood cholesterol promotes tumor growth and metastases (12–14). Choline is also elevated in tumor cells, and is metabolized in the large intestine into pro-inflammatory compounds that may promote cancer development (15–17). So How Many Eggs Are OK to Eat? Given this research, my recommendation for egg consumption is to refute the message that eggs can be eaten liberally. The research strongly supports that the cholesterol, saturated fat and choline in eggs promotes disease, so my recommendation is to keep egg consumption to a minimum. If you are currently living with diabetes, cardiovascular disease or cancer OR if your parents lived with diabetes, cardiovascular disease or cancer, limit your intake of eggs to less than 2 per week. If you are an active individual with no family history of diabetes, cardiovascular disease or cancer, you can eat up to 3 eggs per week. If you’re a night owl, you might be interested to know that your late-night eating habits could impact your health — and not in a good way. Pretty much everyone at one point or another has had a late dinner or indulged in some snacking while watching television or catching up on the day’s work. Some people don’t sleep well at night and may turn to food to try to help them catch some shut-eye. While staying up until the wee hours and noshing may be a routine for you, it might be time to take a second look at these habits that perhaps aren’t so healthy.
Eating late at night: Can affect your weight. Contrary to popular belief, eating late at night doesn’t necessarily mean that you’ll gain weight. What dictates weight gain is how many calories you consume over the course of the entire day, not necessarily when you consume those calories. However, you could end up gaining weight based on the types of foods you may be reaching for as you catch up on Game of Thrones. Potato chips, cheese and crackers, ice cream, cookies… all of these are calorie-laden treats that are surefire ways to pack on the pounds compared to snacks that you might choose during the day: fruit, yogurt, nuts, etc. In addition, it’s easy to go overboard with food portions at night, especially when you get caught up in television or work. Mindless eating kicks in and before you know it, you’ve polished off that bag of Doritos. Can impact your blood sugars. What and how much you eat can directly affect your blood sugars both overnight and the next morning, especially if your snack choices are mostly carbohydrate foods, like crackers, chips, or fruit. Your diabetes medicine may not completely “cover” excessive eating at night and you may be unpleasantly surprised the next morning when you check your blood sugar and find that it’s higher than desired. There are ways to prevent those morning high readings: Choose lower-carb snacks, such as nuts, lower-fat cheese, raw veggies, or a hard-boiled egg, for example. Some carbohydrate may be OK to eat, such as 15–20 grams-worth (a small piece of fruit or 6 ounces of light-style yogurt, for instance). Otherwise, if you prefer to eat later at night, talk with your doctor about adjusting your medication to better handle late-night eating. Might raise the risk of breast cancer. A new study published in the journal Cancer, Epidemiology, Biomarkers & Prevention shows that nighttime eating may raise the risk of breast cancer, as well as Type 2 diabetes. The authors of the study found that fasting overnight is necessary for overall health and helps the body metabolism work in sync with the body’s sleep-wake cycles. In this study, for every three extra hours of fasting at night, women were 20% less likely to have high blood sugars and a lower risk of illness. Previous research has shown that women with Type 2 diabetes have a 23% higher risk of getting breast cancer; night-shift workers also have a higher risk of breast cancer. Of course, this is a single study, so more work needs to be done in this area. However, it’s certainly food for thought, especially if you’re at risk for getting Type 2 diabetes or breast cancer. Raises the risk for acid reflux. There’s no surprise here: Chowing down after everyone else has gone to bed may seem like a good idea, but there’s a price to pay: heartburn. Lying down after eating (at any time of the day or night) can cause acid from the stomach to “backwash” into the esophagus, causing pain, burning, and shortness of breath. Continued episodes of heartburn may indicate gastroesophageal reflux disease, or GERD, which, if not treated, can lead to further problems over time. If you do eat at night, choose lower-fat, nonacidic foods, watch your portions, and allow at least two hours to pass before lying down. Can affect learning and memory. A study done with mice who were fed when they should have been sleeping showed that they had extreme difficulty in remembering what they had previously learned; they also had trouble with object recognition. Scientists believe the same issues can occur in humans, and it’s based on — again — the disruption of the sleep-wake cycle. Once your internal clock gets messed up, a whole host of problems, including learning and memory troubles, can set in. Tips to deal with midnight munching • Review your schedule and see if you can find a way to get to bed earlier. Consider getting up earlier instead of staying up late. • Distract yourself. If you’re grabbing something to eat because of boredom, go for a walk, read a book, take a bath or better yet…go to bed. • Choose healthier, lower-fat snacks. Try to keep fatty, tempting snacks out of sight (or don’t buy them at all). • If you must eat a late meal or snack, eat it only in the kitchen or dining room, not while working on the computer or watching television. • Don’t skimp on calories earlier in the day. Skipping breakfast and grabbing only a salad for lunch are guarantees that you’ll overeat at night. • Eat plenty of protein and fiber at dinner. Both of these nutrients can fill you up so that you may be less likely to eat later in the evening. Adopted from Diabetes Self Management(Amy Chambell) |

 RSS Feed
RSS Feed
